In Vitro Fertilization (IVF)
Our team offers some of the highest IVF success rates in the nation.
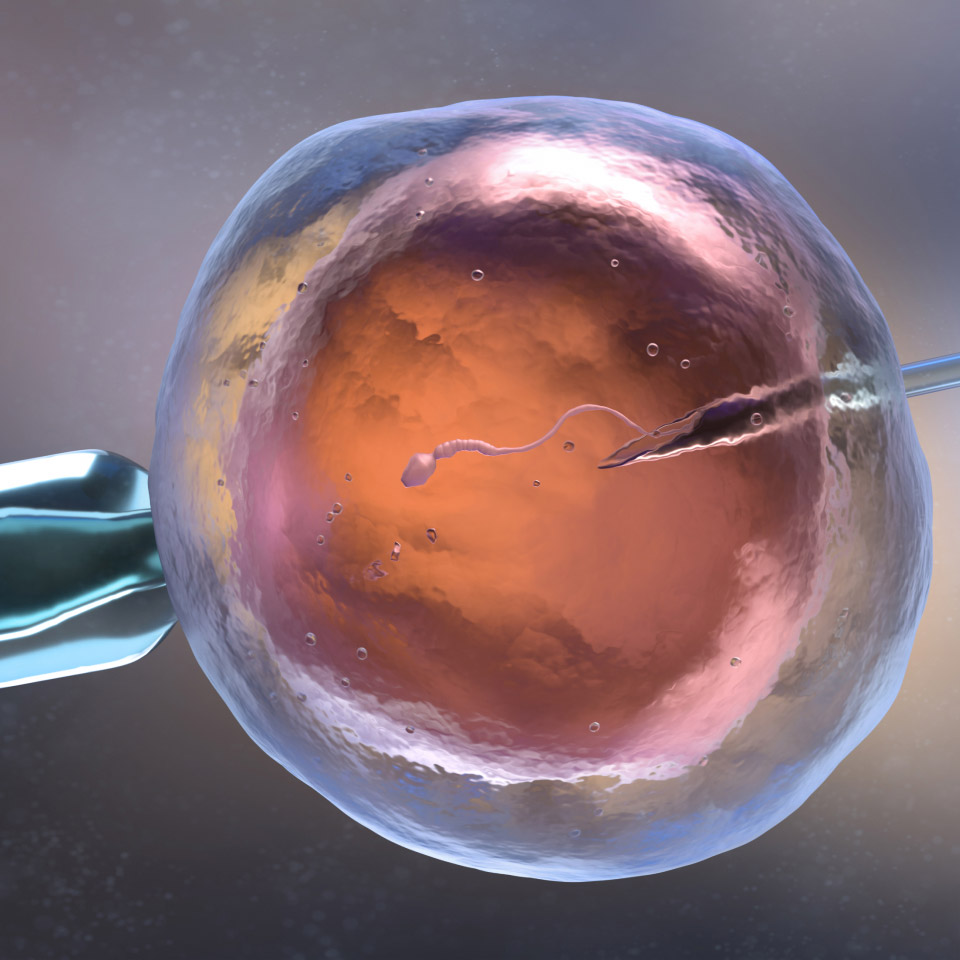
Solving the infertility puzzle can be a long, discouraging process. IVF offers renewed hope. Our staff will make every effort to provide you with the personal and compassionate care you need during your treatment.
How Does IVF Work?
IVF increases the probability of pregnancy by harnessing the body’s own reproductive potential. During a typical menstrual cycle, a hormone called FSH (follicle stimulating hormone) signals to your body to release an egg (oocyte) through a follicle. Typically one egg is released per cycle, but by giving the body more FSH, more of the oocytes can be cultivated in the hope they will generate a fertilized egg, a good embryo, and ultimately a baby.
What Our Patients Are Saying
“IVF and infertility can be incredibly overwhelming. Your staff went beyond my expectations in every way and made me feel taken care of and in good hands. A truly top notch team!”
How Can I Afford IVF Without Health Insurance?
In order to make IVF accessible to everyone, we offer several different treatment plans with special pricing for patients without health insurance. IVF Assist starts at $14,300 (not including medications), and IVF Select starts at $24,500 (also not including medications). We also offer EGG Assist and Frozen EGG Assist for patients who determine that using donor eggs is right for them. You can learn more about financing options available to you, or speak to one of our financial experts to determine the best payment plan for your treatment.
How Much Time Is Required for IVF Treatment?
One of the more nerve-racking aspects of IVF is managing the timing. We work hard, and offer access to multiple locations, to ensure our patients get into the office at the right time in their IVF cycle. Once you and your partner have signed the consent forms for treatment, medications begin. But for those with IVF insurance coverage, insurance company review times can vary from days to weeks.
You will make multiple visits to one of our centers for evaluations, monitoring, and blood work. Once an active treatment cycle begins, you will receive a message on our secure portal with your directions for the next day’s treatment. We understand treatments are a major time commitment and strive to make the process as easy as possible.
Where Do I Begin?
Once you become a patient, we take a detailed history, assess hormonal profiles, do a semen analysis, and examine the uterine cavity and fallopian tubes to diagnose your condition and create a treatment protocol tailored specifically for you.
What Kind of Medications Are Used for IVF?
Three major medication protocols are used to boost your reproductive potential by stimulating your ovaries to make more eggs. Ironically, most of these protocols begin with birth control pills to help stabilize your hormonal profile, minimize miscarriage rate, and provide some control over your cycle.
These protocols also include daily injections under the skin through a very small needle. Next, you will be prescribed a stimulatory medication similar to a hormone your body naturally makes but at a higher concentration. These medications are taken to prepare your body to begin the final egg maturation process and ovulation.
Once your physician determines the eggs are mature, you will be asked to take the ovulatory trigger shot. Approximately 36 hours after this shot, you will go to our Reading, Massachusetts location for an egg retrieval. After the retrieval, you will begin medication to prepare your body for transfer of the embryos.

What Happens During Egg Retrieval?
Once you arrive in our office, you will be sedated so that our physicians can perform the 10-minute procedure of retrieving the egg, using ultrasound to guide them. Once awake, you will be transported to our recovery room for monitoring. When you are discharged, typically after about two hours, we ask that you return home to relax and recuperate.
What Happens to My Eggs?
Within a minute of the procedure, the eggs are transported to the lab where they are examined under the microscope and fertilized. The next day, we will contact you to discuss how the eggs and embryos have fared and set the day for transfer.
What Is the Embryo Transfer Process?
For an embryo transfer, you will return to the Reading center, where your doctor will discuss the progress of your embryos. Then, under ultrasound guidance, your embryo, or embryos, will be guided into the endometrial cavity and placed in a position to maximize successful pregnancy.
When Do We Know If the Embryo Transfer Was Successful?
For some, the final two weeks of the cycle are the most challenging. These days may seem to take forever to pass. Remember, there is little that can influence the fate of the embryos at this stage.
We know the day of the pregnancy test is anxiety provoking, so we work to get these results to you quickly. A welcomed pregnancy is followed carefully with a series of blood tests, measuring the increasing levels of pregnancy hormone. Once we anticipate that we will be able to visualize the pregnancy by ultrasound, we will do so. Medication regimens will change, and we will transition you to assuming care with your obstetrician.
What If It Was Not Successful?
The day of the pregnancy test is not always filled with happiness. The disappointment of a negative test can be paralyzing, if only temporarily. When you are ready, we invite you to make an appointment to meet with your physician to discuss the cycle and what was learned. A negative pregnancy test does not necessarily mean that pregnancy cannot occur; it simply means that it has not happened yet.
Common Questions About In Vitro Fertilization (IVF)
In vitro fertilization (IVF) is a fertility treatment in which eggs are retrieved from the ovaries, fertilized with sperm in a specialized laboratory, and the resulting embryos are transferred into the uterus. IVF may also include embryo freezing or genetic testing, depending on your treatment plan.
IVF may be recommended for individuals or couples experiencing blocked fallopian tubes, male factor infertility, diminished ovarian reserve, unexplained infertility, recurrent pregnancy loss, endometriosis, or unsuccessful treatment with other fertility methods.
IUI places prepared sperm directly into the uterus around ovulation to support natural fertilization. IVF involves fertilization outside the body with embryo transfer afterward. IVF is typically recommended for more complex fertility challenges or when higher success rates are desired.
IVF success rates depend on age, ovarian reserve, embryo quality, diagnosis, and whether donor eggs or genetic testing are used. Success is highly individualized, which is why a personalized consultation is important.
A typical IVF cycle may take 4–8 weeks from evaluation through embryo transfer, though timelines vary depending on testing, ovarian response, embryo freezing, and individualized treatment planning.
Most patients tolerate IVF well, though some parts of treatment, such as hormone injections, monitoring, and egg retrieval, may cause temporary discomfort. Your care team will guide you through every step and help manage expectations.
IVF can include preimplantation genetic testing (PGT) to screen embryos for certain chromosomal abnormalities before transfer. Whether this is recommended depends on age, history, diagnosis, and treatment goals.
IVF costs vary depending on medications, monitoring, genetic testing, embryo freezing, and insurance coverage. Fertility Centers of New England offers financing resources and affordability programs to help patients navigate treatment costs.

