About Fertility
Converting Follicle Stimulating Hormone (FSH)/Intrauterine Insemination (IUI) Cycles to In Vitro Fertilization (IVF)
For many couples, the inability to conceive is caused by abnormal or absent ovulation. Normal ovulation involves the natural recruitment of an egg that has been hibernating in the ovary since before birth. Ovulatory dysfunction is often corrected with hormonal medication which stimulates the ovary to ovulate. The hormone used is follicle stimulating hormone (FSH) which as the name implies is a hormone that stimulates the ovarian follicle. The follicle is a fluid-filled cyst which holds the ovulating oocyte (egg). The FSH stimulation is often combined with an intrauterine insemination (IUI) at ovulation in order to optimize fertilization.
It is important to carefully monitor FSH IUI cycles with dosing adjustments as needed. Monitoring involves checking blood/serum hormonal levels of estrogen (estradiol) as well as ultrasound monitoring of both quantity and size of the maturing follicles which contain the oocytes. The intent of the hormonal stimulation is to enable and optimize the birth of a single healthy child – – not to get twins or triplets. Even with careful (in some cases daily) monitoring, the ovary will produce what is medically deemed to be an excessive number of oocytes. This can be associated with an unacceptably high risk of multiple births. In these cases, the couple will be given the option to cancel the cycle (no sperm – – no triplets) or instead to convert to an in vitro fertilization (IVF) cycle. In an IVF cycle, the follicles are aspirated under ultrasound guidance to retrieve the oocytes. The oocytes are fertilized outside of the body and in a controlled fashion a single embryo can be transferred to the uterine cavity. Any remaining viable embryos of good quality can be cryopreserved.
In September 2005, the Fertility Centers of New England published an abstract looking at our own experience with IUI to IVF conversions (“Should High-Responding Gonadotropin IUI Cycles be Converted to IVF in an Insurance Mandated State?” R.I. Hardy, S. McLellan, K. Delegge, J.A. Hill, L. Scott Fertility and Sterility September 2005 (Vol. 84 Supplement 1, Page S310). The abstract was presented at the annual international meeting of the American Society for Reproductive Medicine. The study reviewed pregnancy rates in high-responding FSH IUI cycles emergently converted to IVF. Four patient groups (divided into > and < 38 y.o.) were analyzed for delivery rates: 1) first time IUI cycles 2) total (1-3) IUI cycles; 3) IUI cycles emergently converted to IVF due to ≥ 5 mature follicles present after stimulation; and 4) first time IVF cycles. The delivery/ongoing pregnancy rates were computed. The data is presented in the table below.
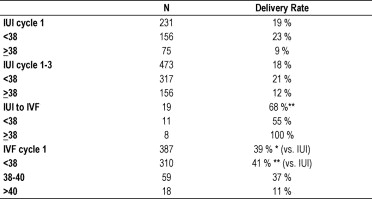
* P<0.01, ** P<0.001
The authors concluded that high-responding FSH/IUI cycles should be converted to IVF. The increased pregnancy rate in this converted group as compared to first time IVF patients also suggests possible effects of patient selection, down-regulation or FSH acclimatization. The favorable pregnancy rates in the converted cycles also prompted re-evaluation of required FSH/IUI treatment prior to IVF approval in insurance mandated states.
If you have further questions or clinical concerns, feel free to speak with your physician regarding treatment options.


