Intracytoplasmic Sperm Injection (ICSI)
Innovation in fertility medicine has empowered couples and given them new hope. If previous IVF cycles have been unsuccessful, intracytoplasmic sperm injection (ICSI) may be a way to overcome your fertility challenges, especially in cases of poor sperm parameters, and renew your sense of hope.
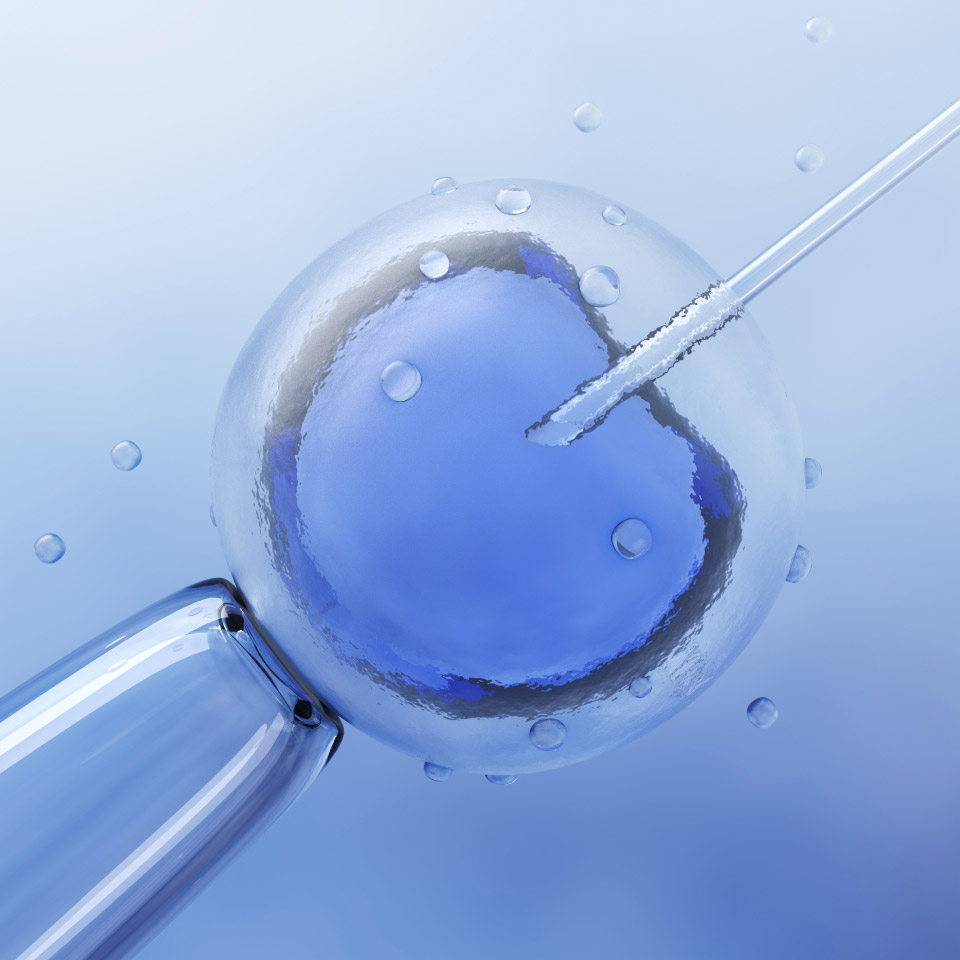
What Is Intracytoplasmic Sperm Injection?
Intracytoplasmic sperm injection (ICSI) is a procedure in which a single sperm is injected directly into an egg harvested during a woman’s IVF cycle. Pronounced “icksy,” this procedure was developed to overcome male fertility problems, but it can also be used to address a number of fertility challenges, including:
- prior fertilization attempts where standard insemination failed
- a low number of eggs were obtained
- the eggs are thought to be of poor quality
- to maximize chances of fertilization during IVF
Success Rates
Many barriers to fertilization can be overcome with this innovative but labor intensive procedure. Success rates and costs vary greatly between different IVF centers. The IVF Laboratory at FCNE has an exceptional fertilization success rate of over 75% and our costs for this procedure are the most competitive in the region.
ICSI is considered a safe and effective therapy for male factor infertility by the American Society of Reproductive Medicine, but may carry an increased risk of passing on genetic abnormalities to children. ICSI is not for everyone, but for those who otherwise could not be parents, ICSI offers another path to achieving a successful pregnancy.

